

Insurance Claims Survey: How Insurers Reduce Calls, Complaints, and Churn

The Insurance Claim is the Moment that defines Customer Loyalty.
In insurance, customers don’t remember the policy.
They remember the claim.
The claim is when stress is highest.
Expectations are urgent.
Patience is limited.
And when the process breaks even slightly, the impact shows up fast:
- Repeat calls to the contact center
- Escalations to supervisors
- Complaints on social media
- Policy cancellations at renewal
If the process feels slow, confusing, or unresponsive, customers remember it.
They call repeatedly. They escalate. They complain.
And sometimes, they quietly switch insurers at renewal.
That’s why more insurers today are investing in insurance claims surveys – not just to measure satisfaction, but to identify friction early.
What is an Insurance Claims Survey?
An insurance claims survey is a short feedback survey sent after key claim interactions to understand what went right, what went wrong, and where the process needs fixing.
It helps insurers quickly identify issues like:
- unclear communication
- delays or confusion in the process
- dissatisfaction with the outcome
- frustration that could lead to repeat calls or complaints
Most insurers run these surveys using structured insurance customer feedback software that automatically sends surveys, analyzes responses, and flags problems that need attention.
To measure the experience, teams typically use three metrics:
- Insurance claims NPS → measures trust and long-term loyalty after the full claim journey
- Post claim CSAT → measures satisfaction at each stage of the process
- CES (Customer Effort Score) → measures how hard or easy it was to file and follow up
→ The goal is simple: detect dissatisfaction before it becomes a churn, a complaint, or a one-star review you never saw coming.
Why NPS Immediately After Claims Matters More Than Most Insurers Think
→ Insurance claims are where customers actually decide to stay or leave
Let’s be honest, most of your customers never really test you.
They pay premiums year after year. They don’t claim. They renew out of habit, out of inertia, sometimes because switching feels like too much effort. You might even think that’s loyalty.
It isn’t.
The moment they file a claim – everything changes. That’s the moment the relationship is actually tested. And the numbers are uncomfortable:
- 80% of policyholders who report a poor claims experience have left or are planning to leave (J.D. Power / Accenture)
- Poor claims experiences put up to $170 billion in global insurance premiums at risk (Accenture)
- 31% of claimants are not fully satisfied with their claims-handling experience, and of those, 30% have already switched carriers (Accenture)
- 87% of policyholders say the claims experience directly impacts their decision to remain with their insurer (EY)
Here’s what makes that even harder: most of those customers won’t tell you they’re unhappy.
Only 1 in 25 dissatisfied customers actually complain. The other 24 leave silently, and you find out at renewal, six to twelve months too late.
And yet, most insurers today still have no structured, real-time way to measure the claims experience. They rely on complaints data, call centre volumes, or anecdotal feedback from branch managers.
None of that gives you the full picture. None of that gives you enough time to act.
That’s exactly the gap a claims satisfaction survey for insurance is designed to close.
A well-designed claims satisfaction survey insurance program helps insurers detect problems early – before dissatisfaction turns into churn.
But only if it is deployed at the right moment.
How Insurers Use SurveySensum to Improve Claims Experience
Most insurers do not struggle with collecting feedback.
They struggle with acting on it fast enough.
And SurveySensum connects feedback directly to action through a structured workflow supported by specific platform features.
Here is how that process actually works in practice.
Step 1: Build the Right Claims Survey in Minutes
You do not need to reuse the same survey for every claim. Each stage in the journey requires different questions and a different purpose.
All you have to do is decide on your use case – submission, delay, approval, rejection, or closure.
Share those details with SurveySensum AI survey builder. And it will automatically create a complete, stage-specific survey.
No manual configuration. No starting from scratch every time.
Along with the survey itself, you also get:
- Built-in logic for different claim stages and outcomes
- Multilingual survey support
- White-label branding for consistent customer communication
→ Operational outcome: Surveys are ready to deploy across teams without manual configuration.
Step 2: Trigger Surveys Automatically at the Right Moment
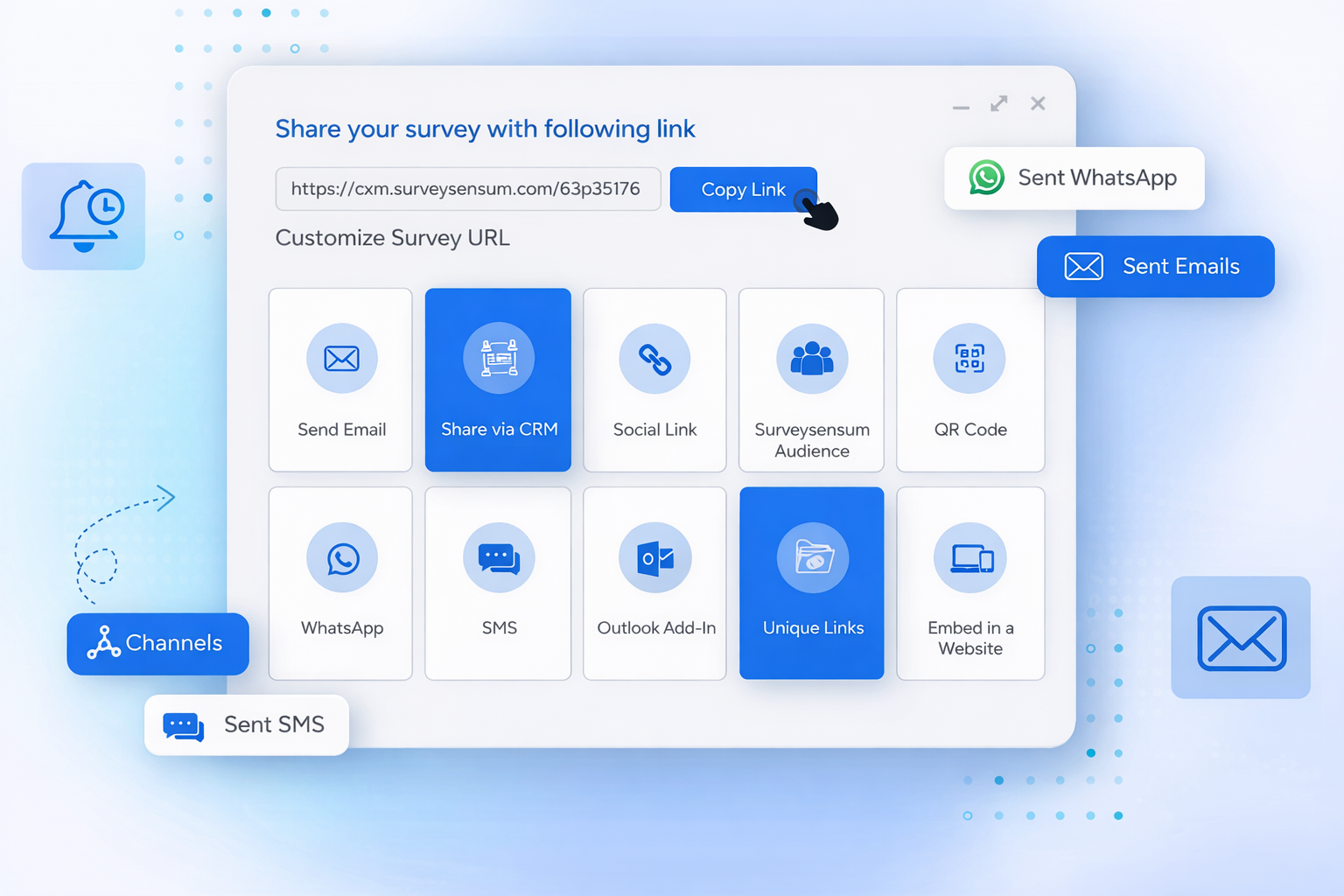
Instead of sending surveys manually, triggers run automatically when a claim event occurs.
SurveySensum supports:
- Event-based survey automation through CRM or workflow integration
- Scheduled and triggered survey campaigns
- Automated reminders to non-responders
- Multi-channel distribution via Email, SMS, WhatsApp, and web links
These capabilities ensure feedback is captured immediately after key claim events.
→ Operational outcome: Feedback is collected at the exact moment to gather in-moment feedback while choosing the channel that delivers high response rate.
Step 3: Monitor Performance Through Role-Based Dashboards

Once responses start coming in, teams need visibility into performance across branches, regions, and claim types.
SurveySensum provides:
- Role-based dashboards with access control
- Hierarchical views for branch, region, and corporate levels
- Performance tracking by handler, claim type, and outcome
- Real-time monitoring of NPS, CSAT, and CES scores
These dashboards ensure every team sees the data relevant to their responsibility.
→ Operational outcome: Managers can quickly identify where performance is declining and where intervention is needed.
SurveySensum’s SensAI chat-based engine gives you instant insights. All you have to do is ask in plain english. No more digging into excel sheets or dashboards.
Why was your NPS low last week? → Get the answers within seconds!
Step 4: Analyze Feedback in Real Time
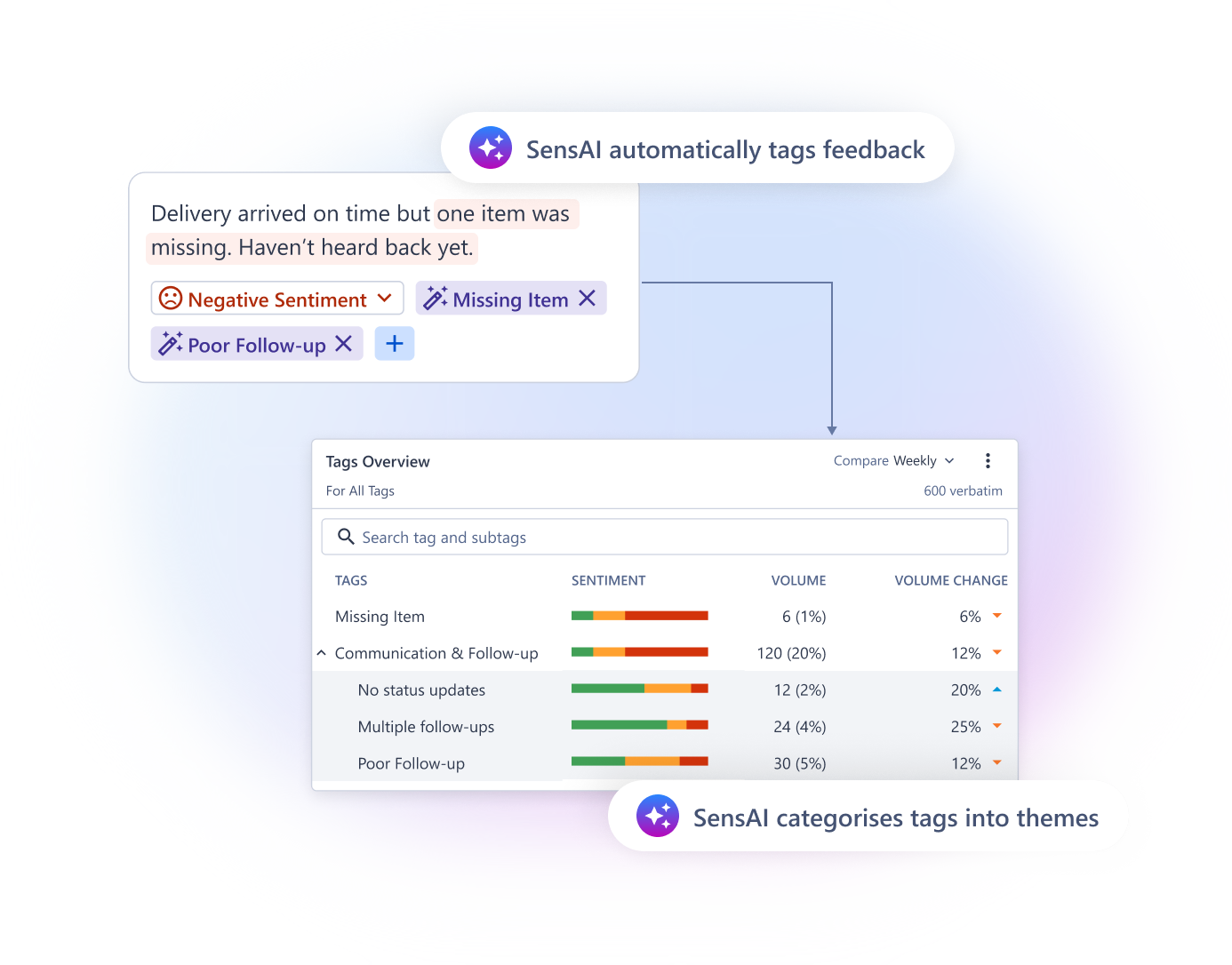
Once responses start coming in, the system converts feedback into clear operational signals.
SurveySensum includes:
- AI-powered text analytics that automatically tags comments into themes
- Historical trend analysis to identify recurring service issues
- Sentiment detection for open-ended responses
These features eliminate manual spreadsheet analysis and surface root causes quickly.
→ Operational outcome: Teams immediately know which claims are generating dissatisfaction, which branches are underperforming, and which issues are recurring.
Step 5: Closed Loop Ticketing System
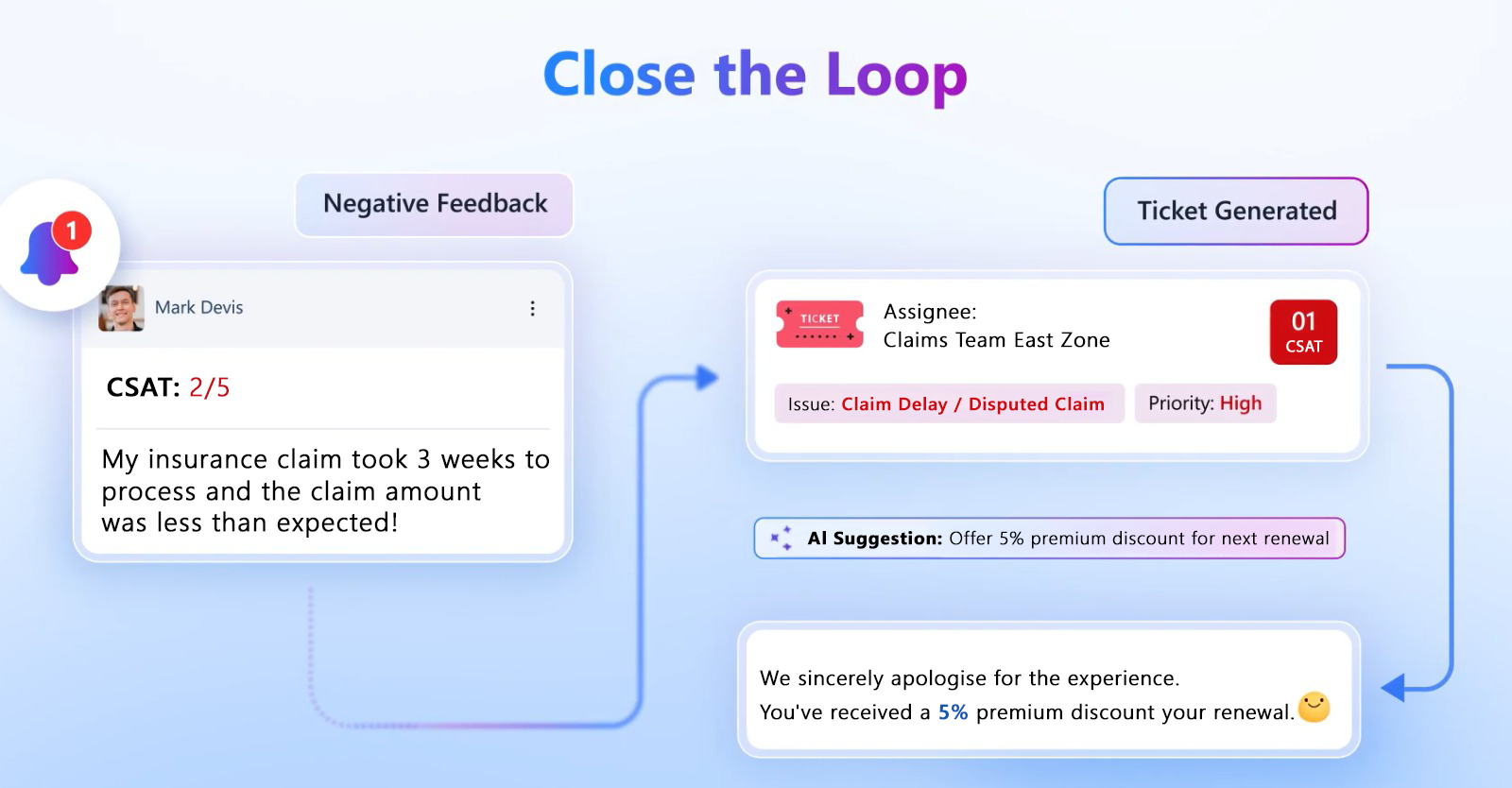
When a customer reports dissatisfaction, the system initiates a response workflow automatically.
SurveySensum offers:
- Instant detractor alerts when low scores are submitted
- Team-based assignment rules based on hierarchy
- Closed-loop ticketing system that creates tickets automatically
- Escalation workflows for high-risk responses
These features ensure every negative experience is routed to the right team immediately.
→ Operational outcome: No dissatisfied customer is missed or ignored.
Step 6: Track Resolution Until Closure
The final step ensures feedback leads to measurable action.
SurveySensum enables:
- Case tracking dashboards to monitor follow-up progress
- Resolution time tracking for SLA compliance
- Automated status updates
- Performance reporting by branch, handler, or claim type
These tools turn feedback into a managed operational process rather than a reporting exercise.
→ Operational outcome: Feedback becomes part of daily operations, not a monthly report.
With this workflow running automatically, teams can finally see where the claims process is breaking.
What an Insurance Claims Survey Actually Helps You Fix
Here are the most common operational issues claims feedback reveals.
1. Communication Gaps
This is the number one driver of dissatisfaction.
Customers don’t necessarily expect instant claim approval.
But they do expect clarity.
Typical feedback sounds like:
- No one updated me about my claim
- I didn’t know what was happening
- I had to call multiple times
- I wasn’t told the next steps
These signals are easy to detect through structured feedback.
2. Processing Delays
Delays are sometimes unavoidable.
But silence makes them worse.
A claims survey helps teams understand:
- where delays occur
- how customers perceive waiting time
- whether expectations were set clearly
This allows operations teams to fix workflow bottlenecks instead of guessing.
3. Documentation Confusion
Many claims require documents.
But customers often struggle with:
- understanding requirements
- submitting the right files
- knowing what is missing
Feedback helps identify:
- unclear instructions
- repeated document requests
- system usability issues
4. Rejection Dissatisfaction
Rejected claims are emotionally sensitive.
Customers want transparency, fairness, and explanation.
A targeted survey after rejection helps insurers understand:
- whether the decision was communicated clearly
- whether customers felt treated respectfully
- whether escalation risk is rising
5. Poor Closure Experience
Even when claims are approved, the experience can still feel stressful.
Common issues include:
- delayed settlement confirmation
- unclear payment timelines
- lack of final communication
A simple post-closure survey helps teams confirm that the journey ended smoothly.
Should Insurers Use NPS, CSAT, or CES After a Claim?
This is one of the most common questions claims and CX teams ask.
And the answer depends on what you want to measure.
| Metric | What It Measures | When to Use |
| CSAT (Customer Satisfaction Score) | Satisfaction with a specific interaction or service step | After individual claim touchpoints |
| CES (Customer Effort Score) | How easy or difficult the process felt for the customer | When evaluating process simplicity or friction |
| NPS (Net Promoter Score) | Trust, loyalty, and likelihood to stay with the insurer | After major claim outcomes or the full journey |
And here’s the practical recommendation
Most insurers benefit from a simple combination:
- CSAT for transaction-level feedback
- CES to identify friction in processes
- NPS to measure loyalty after the claim journey
- One open-ended question to understand the reason behind the score
This combination helps teams detect dissatisfaction early, fix operational issues faster, and reduce churn risk before renewal.
When to Send Surveys in the Claims Journey (The Exact Trigger Points)
This is where most insurers get it wrong. And it’s where your competitors are completely silent.
Here’s exactly when to trigger a claims survey and what to measure at each point:
| Trigger Point | What to Measure | Recommended Metric | Sample Question | Why It Matters |
| After Claim Submission (FNOL) | Ease of filing and clarity of next steps | CES | Was it easy to submit your claim? | Detects early friction that leads to repeat calls. |
| After Claim Registration | Communication clarity and customer confidence | CSAT | Did you receive confirmation quickly? | Confirms customers understand what happens next. |
| During Claim Delay (Beyond SLA) | Frustration and communication gaps | CSAT + open-ended | Were you informed about the delay? | Identifies dissatisfaction before complaints escalate. |
| After Claim Approval | Satisfaction with outcome and explanation | NPS + CSAT | Was the decision explained clearly? | Ensures approval does not leave confusion. |
| After Claim Rejection | Trust and fairness perception | NPS + open-ended | Was the reason for rejection clear? | Highest risk point for churn. |
| After Claim Closure | Overall experience and loyalty risk | NPS + CSAT | How likely are you to recommend us? | Measures retention and renewal intent. |
Best channels to reach your policyholders: Email · SMS · WhatsApp
Different customers respond differently. That’s why flexibility across channels isn’t optional. It’s essential for getting response rates high enough to be meaningful.
Operational insight: An approved claim does not always mean a satisfied customer.
Customers may still feel frustrated when timelines are unclear, updates are missing, or settlement details are not fully explained.
Research shows that communication, transparency, and processing time are among the strongest drivers of claims satisfaction, regardless of whether the claim is approved.
That’s why capturing feedback after approval helps insurers detect hidden dissatisfaction before it turns into repeat calls, complaints, or churn.
Using SurveySensum, insurers automate all six of these triggers across every stage of the claims journey, with no manual follow-up and no missed moments.
👉 See how trigger-based surveys work for insurance claims
Best Questions to Include in an Insurance Claims Survey
A strong survey is short, clear, and focused.
You don’t need 20 questions.
You need the right ones.
Here are practical examples insurers commonly use.
- How satisfied are you with the handling of your insurance claim?
- How would you rate the time taken to process your claim?
- Did you receive timely and clear updates during the claims process?
- How easy was it to submit documents and complete your claim?
- How helpful was the claims representative who handled your case?
- How likely are you to recommend our insurance company based on your claims experience?
- What could we have done better during your claim?
These questions reveal root causes that dashboards cannot detect.
Why do Open-Ended Questions Matter in Claims Surveys? When you add open-ended questions to your insurance claims survey, you start seeing what customers actually experience, not just the score.
Here’s what customers commonly say after a difficult claim:
- “Nobody told me my claim was rejected. I found out after calling three times.”
- “The agent promised a 5-day resolution. It took three weeks.”
- “I submitted the same documents multiple times. Nobody explained what was missing.”
- “My claim was approved, but the settlement amount was lower than expected.”
- “I had to call several times and explain the situation again.”
- “I was told the claim was under review. I still don’t know what’s happening.”
Read those again. Notice what they have in common. Notice the pattern.
Customers are rarely complaining about the decision itself.
They are complaining about:
- lack of communication
- unclear explanations
- repeated effort
These are the patterns they repeat across branches, regions, claim types, and handlers.
The problem is that most insurers only encounter this feedback when it’s already too late: in a formal complaint, a cancellation, or a negative Google review.
With AI-powered text analytics, you can detect these patterns automatically, before any individual complaint becomes a systemic one.
SurveySensum’s AI text analytics tool automatically tags and categorizes open-ended feedback, surfacing recurring themes across handlers, branches, and claim types. So your teams know exactly where to focus.
👉 See how AI Text Analytics detects claims friction from open-ended feedback
How to Break Down Claims Feedback by Branch, Region, and Handler
Here’s the hard truth: an overall claims NPS of 34 tells you almost nothing useful.
It tells you there’s a problem, but it doesn’t tell you where the problem is, who is causing it, or which claim type or channel it’s concentrated in. And without that, you can’t fix it.
This is where most insurers fail. They collect claims feedback, produce a monthly report, and present an aggregate score. Leadership nods. Nothing changes. Customers keep churning.
High-performing insurers do something different. They break claims NPS and CSAT down by:
- Claim type: health, motor, property, life, travel
- Branch or regional office: which locations are underperforming?
- Claims handler or adjuster: who specifically needs coaching or support?
- Channel: digital filing vs. branch vs. call centre vs. agent-assisted
- Claim outcome: approved, rejected, delayed, partially settled
And when they do, here’s what they typically uncover:
- Specific handlers with consistently low scores that aggregate data were masking
- Branches where claim delays are significantly longer than the regional average
- Rejection-related churn concentrated in one particular product line
- Digital claim-filing channels are generating measurably more friction than branch-based ones
That’s the difference between knowing you have a problem and knowing exactly what to do about it.
SurveySensum’s cross-tab analysis enables you to break feedback down by branch, handler, claim type, and outcome. And the SensAI chat-based engine gives you clear answers to operational questions with a single prompt.
👉 See how claims NPS is tracked across branches and handlers
How Claims Surveys Differ by Insurance Type
Claims experiences vary across insurance lines, and so do customer expectations.
That means the timing, questions, and metrics for claims surveys should reflect the specific context of each product.
Here is a simplified comparison.
Claims Survey Triggers and Metrics by Insurance Type
| Insurance Type | Typical Customer Concerns | Key Survey Moments | Primary Metrics | Operational Risk if Missed |
| Health Insurance | Approval delays, reimbursement confusion, repeated document requests | After pre-authorization, claim submission, or reimbursement | CSAT, NPS | Treatment delays, complaints, and trust loss |
| Motor Insurance | Slow inspections, unclear repair timelines, and settlement disputes | After claim registration, inspection, or repair completion | CES, CSAT | Repeat calls, dissatisfaction with repairs |
| Life Insurance | Complex documentation, status uncertainty, and long processing time | After claim submission, verification, or payout decision | CSAT, NPS | Escalations, emotional dissatisfaction |
| Property Insurance | Delayed inspection, unclear damage assessment, and slow settlement | After inspection, processing, or settlement | CES, CSAT | Disputes, negative reviews |
Here’s a practical recommendation.
The survey framework can stay consistent across products, but the trigger timing and focus areas should change based on the claim context.
Tailoring surveys by insurance type helps teams:
- identify issues faster
- improve communication clarity
- reduce repeat calls and complaints
- protect customer trust and retention
With SurveySensum, insurers can configure different survey workflows for each insurance line, ensuring feedback is captured at the right moment for every claim type.
How Claims Feedback Reduces Repeat Calls and Churn
Here’s the operational reality.
When customers feel unheard, they call again.
When they get clarity, calls drop.
Let’s walk through a typical scenario.
| Without Post-Claim Feedback | With Post-Claim Feedback |
| Customer experiences delay → Customer calls support → Agent checks status → Customer calls again
Result:
|
Customer experiences delay → Customer gives low NPS → System triggers alert → Claims manager contacts customer
Result:
|
This is how feedback becomes an operational tool, not just a measurement tool.
We’ve seen this play out across insurers, including Allianz, Prudential, Pramerica Life, and HDFC Life.
👉 Explore how this works for your claims teams
Closed-loop workflows: Turning claims feedback into action
Let’s be direct: feedback without action is useless.
Your customers in claims are already stressed, already frustrated, already questioning whether they made the right choice. In that context, acting slowly is almost as bad as not acting at all.
SurveySensum’s closed-loop ticketing system runs automatically after a low score is received.
That means claims teams can respond faster, reduce repeat calls, and prevent churn before it happens. Here’s what you can do when a low claims score comes in:
1. Detect the risk instantly
The moment a low NPS or CSAT response is submitted, SurveySensum triggers a real-time alert so teams see the issue immediately.
2. Create a ticket automatically
SurveySensum’s built-in ticketing system automatically converts negative feedback into a structured case. No manual tracking. No missed follow-ups.
3. Assign ownership to the right team
Tickets are routed automatically to the responsible person, such as the claims manager, service team, or regional lead, based on predefined workflows.
4. Contact the customer quickly
Teams reach out within a defined SLA while the issue is still fresh. Early contact helps rebuild trust before frustration escalates.
5. Resolve the issue based on clear signals
SurveySensum surfaces the root cause from feedback comments, helping teams address common problems such as:
- claim decision clarification
- missing documentation
- payment timeline confusion
- communication gaps
6. Track resolution until closure
Every ticket remains visible in the system until it is resolved. SurveySensum monitors follow-ups, escalations, and closure status so no dissatisfied claimant falls through the cracks.
7. Close the loop with the customer
Once the issue is resolved, teams confirm closure and ensure the customer feels heard. This final step often determines whether a customer stays or leaves.
What This Looks Like in Practice
A customer submits frustrated feedback on Tuesday morning.
By Tuesday afternoon, they received a call from their claims handler.
“We saw your feedback. We want to make this right. Here’s what we’re going to do.”
That moment does not just resolve the issue. It rebuilds trust.
SurveySensum enables automated closed-loop workflows – ensuring every negative claims experience is assigned, tracked, and resolved. No manual chasing. No missed follow-ups.
What to Look for in Insurance Claims Survey Software
Not every survey tool is built for claims workflows.
Focus on capabilities that help teams act on feedback, not just report it.
Key Capabilities to Evaluate
- Trigger-based surveys: Send surveys automatically after claim events such as submission, delay, approval, rejection, or closure.
- Real-time alerts: Detect low scores instantly and notify the right team for follow-up.
- AI text analytics tool: Analyze open-ended feedback to identify recurring complaints and emerging issues.
- Branch and handler-level dashboards: Break down scores by region, branch, claim type, and individual handler.
- Closed-loop workflows: Create tasks, assign ownership, and track resolution until the issue is closed.
- Multi-channel distribution: Collect feedback through Email, SMS, and WhatsApp to improve response rates.
- Fast implementation: Launch quickly without heavy IT dependency or long setup cycles.
Choosing the right insurance customer feedback software determines whether feedback drives action or just reports. It should support automation, visibility, and action.
👉 See how insurance teams run trigger-based claims surveys with SurveySensum
Why Insurers Use SurveySensum for Post-Claim Feedback
Insurance teams choose SurveySensum because it helps them turn feedback into action, not just reports.
Instead of collecting scores and reviewing them weeks later, teams can respond immediately when a customer signals dissatisfaction.
Here’s what makes that possible:
- Automated surveys are triggered at every key claim event
- Multilingual surveys improve response rates and data quality
- AI text analytics identifies recurring complaints instantly
- Built-in ticketing system assigns issues to responsible teams
- Role-based dashboards track performance across claims operations
- Fast implementation without heavy IT or setup delays
The result is simple.
Issues are detected earlier. Responses are faster. Customers stay.
So, if your team wants to:
- reduce claim-related complaints
- improve communication
- lower repeat call volumes
- identify churn risk early
A structured claims feedback program can make a measurable difference.
SurveySensum helps insurers capture feedback at the right moments, understand root causes, and act quickly – so the claims experience becomes smoother for both customers and operations teams.
Book a demo to see how post-claim feedback workflows work in practice.
FAQs on Insurance Claims Surveys
An insurance claims survey is a feedback questionnaire sent after key claim events such as submission, delay, approval, rejection, or closure to measure customer satisfaction, identify service gaps, and reduce churn risk.
Insurers should send a claims survey immediately after key claim events, such as claim submission, delay, approval, rejection, or closure, while the experience is still fresh.
Low NPS after claims is most commonly caused by:
- delays in claim processing
- poor communication
- unclear claim decisions
- lack of status updates
Claims feedback reduces repeat calls by identifying dissatisfaction early, allowing teams to resolve issues before customers feel the need to contact support again.
Yes. Claims feedback can be tracked by branch, region, claim type, or handler, helping teams identify where problems are occurring and take targeted action.
Most insurers use CSAT to measure satisfaction with individual claim interactions and NPS to measure trust and loyalty after claim resolution. Using both metrics provides a complete view of the claims experience.
Ready to Reduce Calls and Churn After Claims?
If your claims process is leading to:
- rising call volumes
- complaints about delays
- low NPS after claims
- customer churn
…it’s time to fix the process at the source.
See how SurveySensum helps insurers capture, analyze, and act on claims feedback across claims teams, branches, and regions.
















